Contact us
Sending Email...
IMPROVING QULITY OF LIFE
Digitalization provides opportunities but also challenges
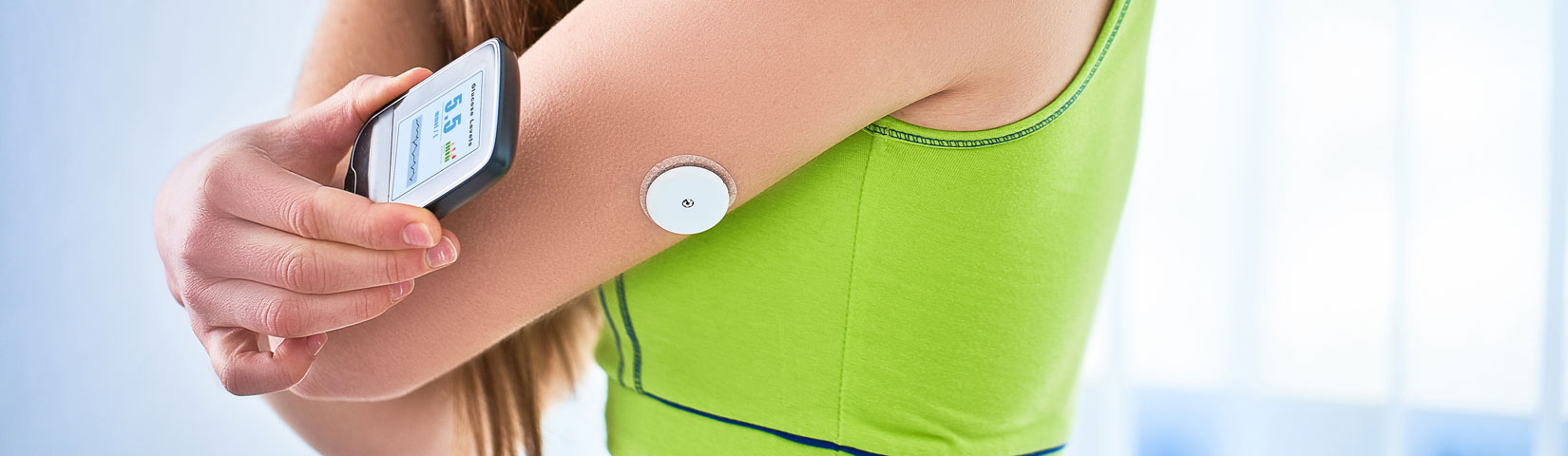
People living with diabetes used to have to prick their finger several times a day to keep track of their blood sugar levels. These days, continuous glucose monitoring offers a vast improvement in quality of life by regularly measuring levels using a sensor underneath the skin. Digitalization of medical devices has created opportunities, but also poses new challenges.
Diabetes is an illness that affects the body’s ability to transform glucose from food into energy for the body’s cells by either entirely or partly stopping the production of insulin. The roughly half a billion people around the world living with diabetes therefore need to constantly check their blood sugar levels to add the correct amount of insulin.
These blood sugar checks used to be done by the patient pricking their finger several times a day to determine what the insulin dose should be. Nowadays, this process has been replaced for many by sensors that send a signal to an automatic insulin pump.
These sensors are put in place with a simple needle prick and can then be worn for weeks or even months. And they are also so small that patients often forget they have them on their body. The insulin pumps, too, have now become so small and simple that they are barely noticed.

Digitalization of medical devices has resulted in better quality of life for many people living with diabetes.
Improving patients’ quality of life
Modern diabetes technology is largely about improving quality of life for patients. Digitalizing sensors and insulin pumps allows patients to easily keep on top of things and make sure everything is working. Data can be presented in real time via the patient’s smartwatch or mobile phone, which can also alert them if their values fall outside permitted levels.
Forwarding the data also keeps the patient’s care team in the loop, for example so they can support patients who are unable to get to a care provider themselves. The significance of this was felt particularly during the Covid-19 pandemic. When patients were unable to visit their doctor, the systems were able to share important diabetes data during virtual healthcare meetings.
Technical innovations in sensors and insulin pumps have meant challenges for medtech companies and their suppliers to continually come up with new and improved solutions.
“One of the challenges is to constantly make the products smaller, which often requires a product’s various components to be able to carry out several tasks simultaneously,” explains Bill Torris, who heads up Nolato’s Technical Design Center in North America.
Seal, protect and release
“Take gaskets, for instance; previously, the material was chosen solely because of its sealing properties. In modern medical devices that are packed with electronics, the gaskets have to be made from materials that provide a seal from liquids, release signals from antennas and protect the electronics from interference from electromagnetic radiation. And when we injection-mold silicone around a battery, for example, the material has to both protect the battery physically and conduct electricity to enable the battery to be charged via induction.
“At Nolato we have the ability to customize our own silicone material and give it precise properties,” says Bill. “This means, for instance, that we can control whether the material conducts or doesn’t conduct electricity, whether it insulates against or conducts heat away from the unit and whether or not it shields against electromagnetic radiation.”
Medical device digitalization poses numerous challenges, but Nolato is better equipped than most thanks to its extensive experience of integrating electronics into products.
“For over 25 years now, Nolato has been integrating mechanical components and electronics into mobile phones and other handheld consumer electronics,” notes Bill. “So using that experience and know-how to digitalize medical devices isn’t new or unusual for us.”
- Medical Solutions
- Medical Devices
- Nolato
- Nolato Magasin
You might also be interested in
SUSTAINABLE DEVELOPMENT
Creating sustainable solutions
INDUSTRY
Medical Devices
STORIES